Prospective Trial of Customized Adherence Enhancement
Plus Long-Acting Injectable Antipsychotic Medication
in Homeless or Recently Homeless Individuals With
Schizophrenia or Schizoaffective Disorder
ABSTRACT
Background: Treatment nonadherence in people with schizophrenia is associated with relapse and homelessness. Building on the usefulness of long-acting medication and our work in psychosocial interventions to enhance adherence, we conducted a prospective uncontrolled trial of customized adherence enhancement (CAE) plus long-acting injectable antipsychotic (LAI) using haloperidol decanoate
in 30 homeless or recently homeless individuals with
DSM-IV–defined schizophrenia or schizoaffective disorder.
Method: Participants received monthly CAE and LAI (CAE-L) for 6 months. Primary outcomes were adherence, as measured by the Tablets Routine Questionnaire, and housing status. Secondary outcomes included psychiatric symptoms, functioning, side effects, and hospitalizations. The study was conducted from July 2010 to December 2012.
Results: The mean age of participants was 41.8 years (SD = 8.6); they were mainly minorities (90%, n = 27 African-American) and mainly single/never married (70%, n = 21). Most (97%, n = 29) had past or current substance abuse and had been incarcerated (97%, n = 29). Ten individuals (33%) terminated the study prematurely. CAE-L was associated with good adherence to LAI (at 6 months, 76%) and dramatic improvement in oral medication adherence, which changed from missing 46% of medication at study enrollment to missing only 10% at study end (P = .03). There were significant improvements in psychiatric symptoms (P < .001) and functioning (P < .001). Akathisia was a major side effect with LAI.
Conclusions: While interpretation of findings must be tempered by the methodological limitations, CAE-L appears to be associated with improved adherence, symptoms, and functioning in homeless or recently homeless individuals with schizophrenia or schizoaffective disorder. Additional research is needed on effective and practical approaches to improving health outcomes for homeless people with serious mental illness.
Trial Registration: ClinicalTrials.gov identifier: NCT01152697
J Clin Psychiatry 2013;74(12):1249–1255
© Copyright 2013 Physicians Postgraduate Press, Inc.
Submitted: December 13, 2012; accepted March 14, 2013 (doi:10.4088/JCP.12m08331).
Corresponding author: Martha Sajatovic, MD, Departments of Psychiatry and Neurology, University Hospitals of Cleveland, 11100 Euclid Ave, Cleveland, OH (martha.sajatovic@uhhospitals.org).
While psychotropic medications are a cornerstone of treatment for individuals with schizophrenia, rates of nonadherence can exceed 60%.1–3 Poor adherence is associated with homelessness.4–6 A review in homeless persons found that the weighted average prevalence of schizophrenia in homeless individuals is 11% and that approximately half of these individuals are not receiving treatment.6 Because a major obstacle to medication adherence is difficulty with medication routines,1,7 long-acting injectable antipsychotic (LAI) medication can be an attractive treatment option. However, LAI is underused for schizophrenia,8 and less than 1 in 5 individuals with nonadherence receive LAIs.8
Building on our work in psychosocial interventions to enhance adherence,9,10 we conducted a trial of customized adherence enhancement (CAE) plus LAI antipsychotic (CAE-L) in 30 homeless or recently homeless individuals with schizophrenia and schizoaffective disorder. We anticipated that CAE-L would be associated with reduced rates of homelessness, improved adherence, and reduced psychiatric symptoms.
METHOD
This was a prospective, uncontrolled trial of CAE-L in nonadherent homeless or recently homeless individuals with schizophrenia or schizoaffective disorder. CAE-L was administered monthly over 6 months. Primary study outcomes were medication adherence, as measured with the Tablets Routine Questionnaire (TRQ),11,12 and housing status. Secondary outcomes included psychiatric symptoms, functioning, side effects, hospitalizations, and treatment satisfaction. Posttreatment follow-up was conducted at 9 and 12 months.
Study Population
Study participants were ≥ 18 years of age, with a DSM–IV diagnosis of schizophrenia or schizoaffective disorder confirmed with the Mini-International Neuropsychiatric Inventory.13 Individuals were recruited from homeless shelters, community mental health clinics, and the community. The study was approved by the local institutional review board, and oversight included an external data and safety monitoring board. All participants provided written informed consent. Individuals had poor adherence (missing 20% or more of prescribed medication) as measured by the TRQ and were currently homeless or had been homeless within the past 12 months as per the Federal definition of homelessness.14 Participants had to be willing to take LAI.
Individuals were excluded if they had known contraindication to haloperidol, were on LAI at screening, had prior treatment with clozapine, had substance dependence, had unstable medical conditions, or were at high risk of harm to self or others. Individuals already in permanent supported housing that included comprehensive mental health services were excluded, and the study was conducted from July 2010 to December 2012. The study is registered with ClinicalTrials.gov (identifier: NCT01152697).
CAE-L Intervention
Long-acting injectable antipsychotic. Haloperidol decanoate was chosen as the LAI, given its low cost and potential generalizability. Individuals already on oral haloperidol treatment were switched to LAI as per the manufacturer’s package insert.15 Individuals not on any antipsychotic treatment or on treatment with antipsychotics other than haloperidol at screening were started on oral haloperidol (2 mg twice daily) and then transitioned to LAI within 2 to 3 weeks of enrollment. Individuals received LAI every 4 weeks for the duration of the study. Subsequent dose modification was based on clinical status.
Customized adherence enhancement. Customized adherence enhancement, originally designed for nonadherent bipolar patients,9,10 targets key areas also relevant to nonadherent individuals with schizophrenia and includes psychoeducation focused on medication, developing medication routines, communicating with providers about benefits and burdens of medications, and managing adherence in the context of substance abuse. Detailed information on CAE is described in greater detail elsewhere.9,10
Modifications of CAE for use in individuals with schizophrenia included reducing the duration of sessions (generally ranging from 30–40 minutes), repetition of key messages, either completing only half of the material from a session that would have been covered with bipolar patients or repeating the material a second time in 2 consecutive sessions to reinforce the key points, and increasing the overall number of sessions (8 sessions, generally given at 1-month intervals on the day that LAI was administered).
Concomitant Treatments
Antipsychotic drugs other than haloperidol were discontinued. Stable doses of psychotropic drugs other than antipsychotics were continued through the course of the study. New psychotropic medications were strongly discouraged. Medications for side effects were given at the discretion of the treating psychiatrist.
Study Assessments
Individuals completed assessments at screening (time of oral antipsychotic drug initiation), at CAE-L baseline (first administration of LAI or first CAE session), and at 13- and 25-week follow-up. All study participants received nominal financial compensation for research assessments but did not receive compensation for other components of study participation.
Primary Outcomes
Primary outcomes were change from screening on the TRQ11,12 and on housing status. Housing status was grouped in progressively less desirable order: permanent housing without assistance, permanent housing with some assistance, transitional housing, short-term/emergency shelter, outdoors, and incarceration. The TRQ format was modified slightly to document adherence values as an exact proportion.
Secondary Outcomes
Adherence was also assessed with the Morisky Rating Scale16 and observed injection frequency of LAI (proportion of injections given within 7 days of the scheduled time). Adherence attitudes were assessed with the Attitude Toward Mood Stabilizer Questionnaire,12,17 which was slightly adapted to include all prescribed psychotropic medication, and the Drug Attitude Inventory (DAI).18
Secondary outcomes included health resource use (hospitalizations) and psychiatric symptoms as assessed by the Brief Psychiatric Rating Scale (BPRS),19 Positive and Negative Syndrome Scale (PANSS),20 and the Clinical Global Impressions scale (CGI).21 Functioning was measured with the Social and Occupational Functioning Assessment Scale (SOFAS).22 Satisfaction with CAE-L was assessed at the conclusion of the 6-month treatment period.
All outcome assessments were conducted at screening, baseline, week 13, and week 25, except for satisfaction with treatment, PANSS, and life and work functioning, which were conducted at the baseline and week 25 visits. After the 25-week treatment, participants continued to receive care in their community mental health clinics or indigent care organizations, and treatment history was communicated to providers at these sites. We conducted limited posttreatment follow-up at 9 and 12 months, which included the CGI.
Safety Measures
Biological and safety outcomes included body mass index (BMI), vital signs, and laboratory testing. Laboratory testing was conducted at screening and week 25. A 12-lead electrocardiogram (ECG) was assessed at screening. Involuntary movements were evaluated with the Abnormal Involuntary Movement Scale (AIMS),23 Simpson-Angus Scale (SAS),24 and Barnes Akathisia Rating Scale (BARS),25 conducted at screening, baseline, and week 25. Participants were assessed for reported side effects at every study visit.
Data Analysis
Descriptive statistics were calculated for baseline characteristics. We conducted a modified intent-to-treat analysis that included all subjects who received at least 1 dose of LAI or 1 CAE session. Statistical analysis was performed using SPSS software version 20 (IBM Corporation, Armonk, New York). In a first analysis, time-to-event data for LAI dropout were modeled using Kaplan-Meier estimation. A Cox proportional hazard model was then fit on the same time-to-event data, to assess what variables might be affecting dropout. Explanatory variables that were considered included age, gender, and personality disorder. Having antisocial personality disorder was found to be significantly related to hazard rate, with higher hazard for those with antisocial personality disorder. Thus, antisocial personality disorder status was included in subsequent longitudinal mixed models of the BPRS, DAI, and Morisky scales.
Mixed models for BPRS, DAI, and Morisky scales considered time of measurement as a categorical variable at baseline, 13 weeks, or 25 weeks. It was of interest to test whether there appeared to be differences in the factor levels associated with time of measurement, which would indicate that there was indeed change over time in the outcome variables subsequent to CAE-L. A random intercept model was adopted, with antisocial personality disorder status included as an explanatory factor. AR(1) error covariance structures were fit.
RESULTS
Screened and Enrolled Samples
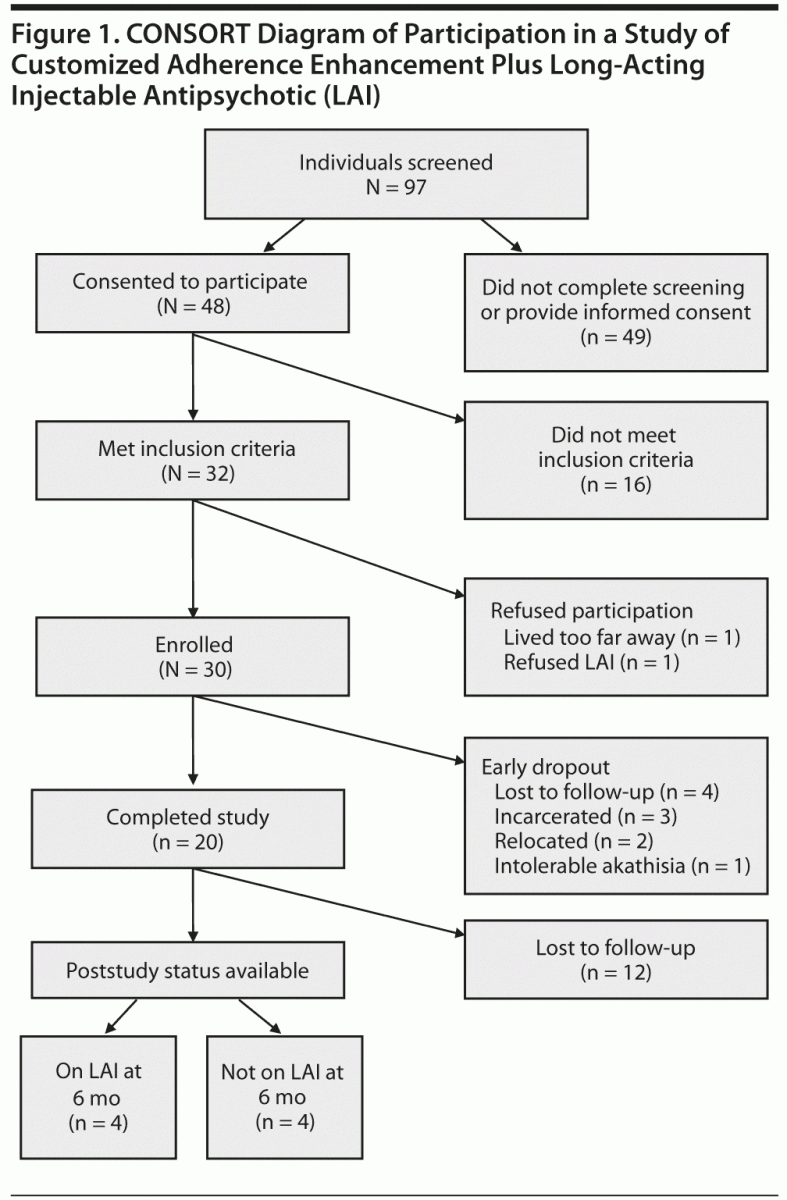
Figure 1 illustrates a CONSORT diagram of participants in the study. Of 97 individuals screened for the study, 48 consented to participate. Among those, 32 individuals met inclusion criteria, and 30 individuals were enrolled. Age, gender, and race did not differ significantly between screened and enrolled patients. Table 1 illustrates demographic and clinical variables in enrolled individuals. Of note were the relatively high proportions of minorities (African-American: n = 27, 90%) and single/never married individuals (n = 21, 70%) and relatively low levels of education (most patients did not finish high school). Nearly all (n = 29, 97%) had a history of past or current substance abuse, and nearly all had past incarceration (n = 29, 97%). In the 6 months prior to study enrollment, participants spent 44% of their time in emergency shelter/short-term housing. On average, individuals missed approximately half of prescribed psychotropic medication.

Long-Acting Injectable Antipsychotic
Injections were administered intramuscularly in the deltoid muscle. Conservative dosing was used to minimize drug-related adverse effects. The mean (SD) endpoint dose of haloperidol decanoate (per monthly injection) was 68.0 (21.1) mg, and the range was 50–100 mg.
Concomitant Medication
Most (n = 25, 84%) individuals were able to identify their prescribed antipsychotic medications at the time of enrollment. Individuals were predominantly prescribed atypical antipsychotics (21 of 25, 84%), with aripiprazole being the most common (6 of 25, 24%). Four of 25 individuals (16%) were on treatment with typical antipsychotics, including 3 taking oral haloperidol and 1 taking perphenazine. Concomitant (nonantipsychotic) medications such as mood-stabilizing drugs (lithium, anticonvulsants) and antidepressants were taken by 9 participants (30%).
Customized Adherence Enhancement Components
On the basis of the results of the standardized adherence needs assessment, 27 of 30 individuals (90%) were assigned to receive the CAE component that addressed inadequate or incorrect understanding of mental disorder (psychoeducation module), 24 of 30 (80%) were assigned to receive the CAE component that addressed lack of medication-taking routines (med routine module), 25 of 30 (83%) received the CAE component that addressed poor communication with care providers (communication module), and 21 of 30 (70%) were assigned to receive the CAE component that addressed substance use (modified motivational interviewing module). Overall, 12 individuals (40%) were assigned to all 4 CAE modules, 14 (47%) were assigned to 3 modules, 3 (10%) were assigned to 2 modules, and 1 (3%) was assigned to a single CAE module.
Dropouts
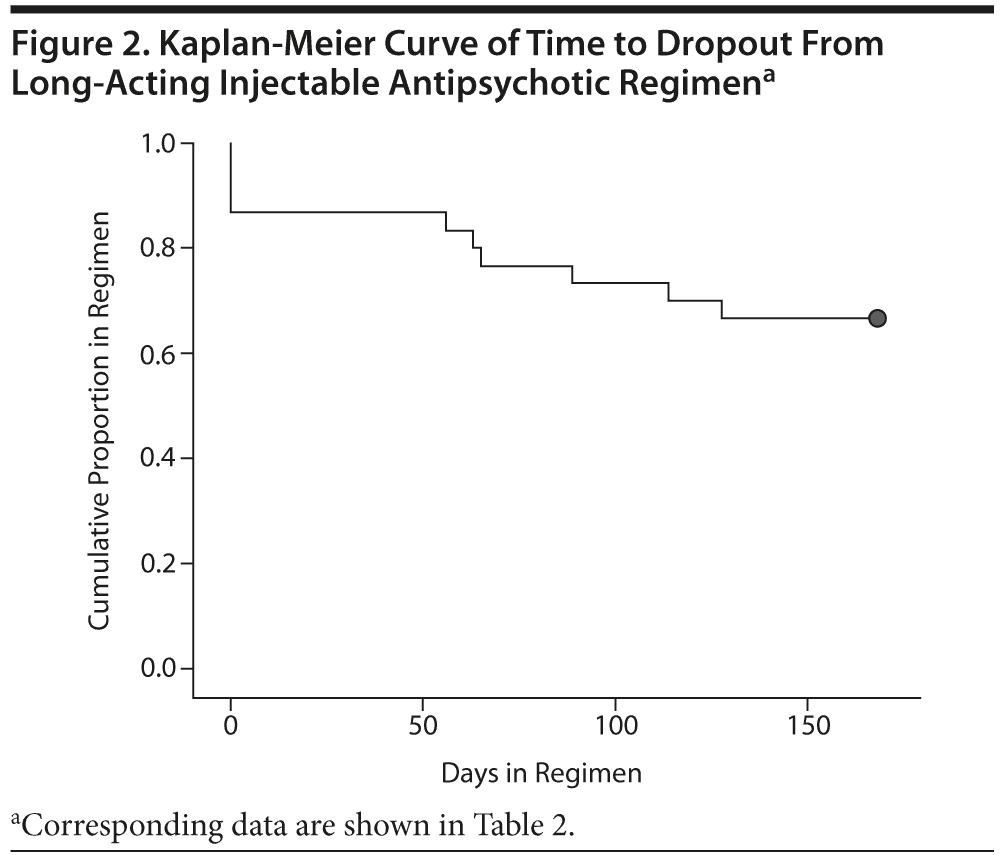
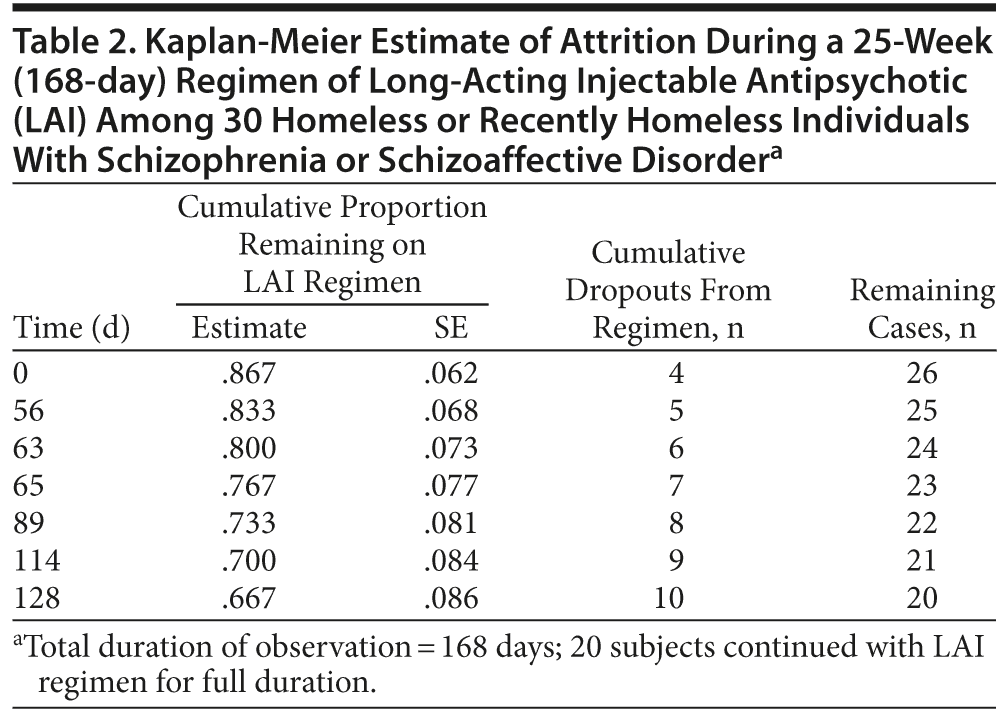
Ten individuals (33%) terminated the study prematurely. Reasons for dropout included the following: 4 (40%) lost to follow-up, 3 (30%) incarcerated, 2 (20%) relocated, and 1 (10%) due to akathisia. Time-to-event data for the dropout from injection treatments were modeled using Kaplan-Meier estimation (Figure 2, Table 2). After 168 days, 66.7% (20 of 30) of individuals completed treatment. Most of the dropout occurred immediately after enrollment, with 13.3% (4 of 30) of subjects dropping out before receiving a single dose of LAI.
Primary and Secondary Outcome Changes
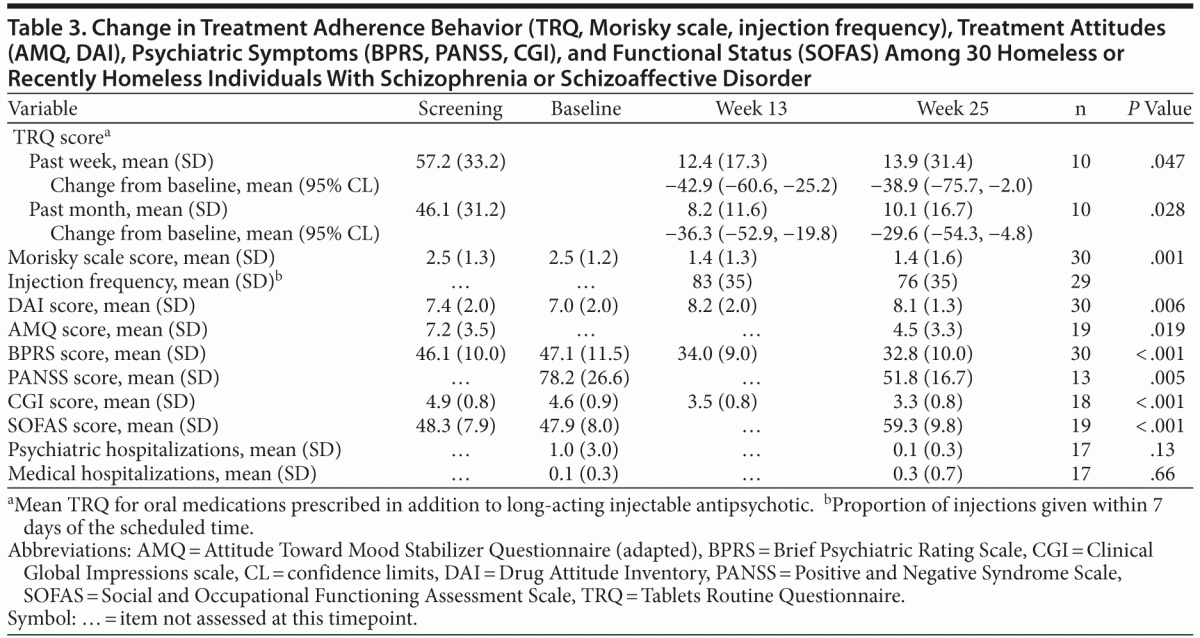
Table 3 illustrates change from screening and baseline in adherence with concomitant oral psychotropic medications, symptoms, housing status, and social functioning, as well as LAI adherence. There were significant differences in scores across time periods for nearly all outcome measures. To evaluate change in housing status, we considered the percentage of days in the past months that were spent in suboptimal housing. A longitudinal mixed model was fit, with time of measurement as a factor, along with antisocial personality disorder status and random subject-level intercept. Age and gender were not statistically significant variables and hence were not included in the reported model. We considered the estimated TRQ means from screening, 13 weeks, and 25 weeks as 56.31%, 39.88%, and 11.82%, respectively. Within the mixed model, the test of equality across time periods had a P value of .001, which supports rejection of the null hypothesis that the time periods have equal means. Hence, these differences are statistically significant. Table 3 also illustrates significant improvement in symptoms (BPRS, PANSS, CGI) and functioning (SOFAS). There were no significant changes in hospitalizations.
Over the course of the study, participants had improvement in housing status. The mean proportion of time in suboptimal housing went from 56% in the 6 months prior to study enrollment to 41% in the first 3 months of the study and 14% in the last 3 months of the study (P = .001).
Although the overall number of individuals with schizoaffective disorder was too small to conduct any comparative analysis, we did note that 13 of the 20 individuals with schizoaffective disorder completed the study and that overall change from baseline in TRQ, DAI, and BPRS scores among individuals with schizoaffective disorder all suggested change in the same direction as was seen in the larger sample. The TRQ and DAI scores, available only for a partial group of the patients with schizoaffective disorder, showed numeric but not statistically significant change. For the BPRS, statistically significant change from baseline was observed among patients with schizoaffective disorder (mean [SD] baseline BPRS score = 44.7 [10.4], mean [SD] endpoint BPRS score = 34.1 [9.9]; t11 = 2.51, P = .029).
Tolerability and Adverse Effects
Table 4 illustrates side effects experienced by > 5% of study participants. Side effects were generally mild to moderate in intensity and transient, except for akathisia, which persisted for some individuals in spite of adjunct therapies. One individual discontinued LAI due to severe akathisia. Another individual had an increase in QTc interval on ECG from 443 milliseconds at baseline to 462 milliseconds on oral haloperidol, and this individual was not started on LAI therapy. The patient’s QTc interval decreased to less than 450 milliseconds when oral haloperidol was discontinued.

With respect to standardized involuntary movement and neurologic rating scales, there were no significant changes in AIMS and SAS scores, but change in BARS scores was significant (P = .019), reflecting the emergence of akathisia. BMI and total cholesterol did not change significantly. There was statistically significant worsening in serum triglycerides (P = .026), but since participants were not fasting prior to blood draws, clinical significance of nonfasting triglyceride changes is questionable.26
There were 5 serious adverse events (SAEs) during the study: 1 emergency room visit for non–study- related medical reasons, 1 hospitalization for non–study-related medical reasons, 1 hospitalization due to seizure and allergic reaction to anticonvulsant medication, and 2 hospitalizations due to suicide attempts. The seizure occurred in an individual with epilepsy, who was nonadherent with prescribed anticonvulsant medication. It is possible that the LAI contributed to the SAE by lowering seizure threshold. Both individuals with suicide attempts were continued on LAI therapy after the attempt and appeared to have a good response to continued exposure to CAE-L. External data and safety monitoring board review of the 2 suicide attempts concluded that they did not appear related to study involvement.
In general, participants expressed satisfaction with CAE-L. The majority strongly agreed (11 of 18, 61.1%) or agreed (7 of 18, 38.9%) that CAE was useful and either strongly agreed (6 of 18, 33.3%) or agreed (10 of 18, 55.6%) that the benefit exceeded the burden or hassle of participation. No individuals discontinued the psychosocial component of the study due to adverse effects.
Posttreatment Follow-Up
Of the 20 individuals who completed 25 weeks of CAE-L, 12 provided information at 3 months poststudy, and 8 provided information at 6 months poststudy. As noted in Figure 1, only 4 individuals out of the 8 with available data continued to take LAI at 6 months poststudy. While CGI scores of those who were still receiving LAI after 25 weeks did not appear markedly different from the scores of those who were not, the small sample size did not permit valid statistical comparison.
DISCUSSION
This prospective, uncontrolled study in homeless or recently homeless seriously mentally ill individuals found that use of a novel psychosocial intervention plus LAI was associated with improvements in adherence and psychiatric symptoms. While there are substantial limitations to the study methods, including small sample size, lack of a control group, and relatively short duration, the findings are still of substantial clinical relevance given the tremendous personal and societal burden related to homelessness among people with schizophrenia.27–29 Approximately 1 in 10 homeless individuals has schizophrenia,6 and there are few established treatments for this vulnerable group.27 The prognosis for these individuals is typically poor, with mortality rates 4 times that of the general population30 and double that of non-homeless individuals with schizophrenia.31,32 Consistent with the multiple challenges faced by homeless individuals with schizophrenia,33,34 the sample enrolled in this study had few social supports, limited education, frequent comorbid substance use, and a history of multiple involvements in the criminal justice system.
Similar to other reports,35 individuals in this study reported missing 46%–57% of prescribed medication. Use of CAE-L was associated with good adherence to maintenance LAI (76% at 6 months) and dramatic improvement in oral prescribed drug adherence, which changed from missing approximately 46% of prescribed medication to missing only 10% of prescribed medication by the end of the study. This could be particularly important for individuals with schizoaffective disorder, who are often receiving multiple psychotropic agents.36 It is not entirely clear what factors facilitated the improved oral adherence, but it is possible that LAI and CAE had synergistic effects on improving insight and acceptance of medications more broadly.
Improvements in psychiatric symptoms have been noted as an independent effect of CAE,9,10 and pairing CAE with LAI may have facilitated further reduction in symptoms and possibly improved insight into need for treatment. Housing improvement is a complicated issue that could have been affected by a variety of factors and may not have been related to CAE or LAI. However, it is also possible that being less symptomatic and better able to manage one’s own personal affairs, such as meeting with social workers, could have helped individuals to obtain appropriate housing.
Both the original version of CAE,9,10 developed for people with bipolar disorder, and the version used in this study consist of detailed manuals that stress pragmatic problem-solving specifically focused on adherence relevant to the individual. Other features included delivering information in small chunks and using modest incentives (ie, washcloths, pencils, pill minders) for active participation.
A recent review suggested that LAIs reduce risk of relapse when combined with psychosocial interventions.37 Use of LAIs reduces the chance that individuals will miss prescribed medication doses due to forgetting or not wanting to take them in situations that can be stigmatizing (such as at work or school). When individuals miss an injection, visit staff can follow up and both assess clinical status and reschedule the injection. LAIs can minimize antipsychotic withdrawal symptoms resulting from partial adherence.38 In addition, LAIs are not influenced by first-pass metabolism, decreasing the potential for drug-drug interactions, and the slow rate of absorption of LAIs may reduce the differences between peak and trough plasma levels,39 resulting in fewer side effects (an important predictor of adherence) relative to oral antipsychotics.40,41 A number of antipsychotic medications are currently available in LAI form, including typical and atypical drugs.37 Newer LAI antipsychotic formulations have relatively low extrapyramidal side effect profiles.37 In our study, in spite of modest haloperidol dosages, akathisia was relatively common and at times not well controlled even with supplemental treatments.
A limitation to study generalizability was the fact that the majority of individuals did not remain on LAI therapy after the study. Perhaps using an atypical antipsychotic with a lower propensity for akathisia could have improved long-term LAI adherence. Additionally, logistic barriers to coordination between community mental health clinic and study staff in transitioning stable individuals to maintenance care and a lack of the CAE/psychosocial component in routine clinical settings could have caused individuals to drop out of care. While CAE-L appears to engage and stabilize this very high-risk group, it may be that long-term or “booster” sessions are needed to maintain these gains.
Given methodologic limitations, it is not possible to conclude that combining CAE with LAI has an additive or synergistic effect. With the relatively severe symptoms and difficulties in concentration and attention experienced by many individuals in the study, it seems unlikely that CAE alone would have been enough to change health outcomes. One could argue that improvement was due to LAI. However, since some of the individuals had been on LAI in the past and were nonadherent, it might be reasonable to expect that a needs-based psychosocial intervention could enhance gains from somatic therapy. Given that few established effective approaches exist to help homeless individuals with schizophrenia, there is a clear need for research that tests effective and practical approaches to improving health outcomes for these vulnerable individuals. In spite of the noted limitations of our study, the findings have substantial implications for clinical practice. If the findings can be replicated under controlled conditions, this could represent a potential new best practice for the treatment of homeless, nonadherent individuals with schizophrenia and schizoaffective disorder.
Drug names: aripiprazole (Abilify), clozapine (Clozaril, FazaClo, and others), haloperidol (Haldol and others), lithium (Lithobid and others).
Author affiliations: Department of Psychiatry (Drs Sajatovic, Levin, Ramirez, and Hahn; Mr Bialko; and Mss Cassidy, Fuentes-Casiano, and Williams), Department of Neurology (Dr Tatsuoka), and Neurological and Behavioral Outcomes Center (Drs Sajatovic and Tatsuoka), Case Western Reserve University School of Medicine, University Hospitals Case Medical Center, Cleveland, Ohio.
Potential conflicts of interest: Dr Sajatovic has received grant support from AstraZeneca, Pfizer, Merck, and Ortho-McNeil Janssen; received royalties from Springer Press, Johns Hopkins University Press, and Oxford Press; and served as a consultant for Cognition Group, ProPhase, and United BioSource Corporation (Bracket). Dr Ramirez has served as a speaker for Bristol-Myers Squibb, Merck, and Novartis. Drs Levin, Hahn, and Tatsuoka; Mr Bialko; and Mss Cassidy, Fuentes-Casiano, and Williams report no conflict of interest.
Funding/support: This study was supported by a grant from the Reuter Foundation to Dr Sajatovic. Support for this project was also provided by the Clinical and Translational Science Collaborative (Dahms Clinical Research Unit) National Institute of Health grant number UL1 RR024989.
Previous presentations: Portions of these data were presented at the 13th Annual Congress on Schizophrenia Research, April 3, 2011, Colorado Springs, Colorado, and the 14th Annual Congress on Schizophrenia Research, April 25, 2013, Orlando, Florida.
Acknowledgment: The authors acknowledge Ms Elisabeth Welter, MS, MA, for assistance with preparation of the manuscript. Ms Welter is affiliated with the Department of Neurology, Case Western Reserve University School of Medicine and University Hospitals Case Medical Center. Ms Welter reports no conflict of interest.
REFERENCES
1. Gilmer TP, Dolder CR, Lacro JP, et al. Adherence to treatment with antipsychotic medication and health care costs among Medicaid beneficiaries with schizophrenia. Am J Psychiatry. 2004;161(4):692–699. doi:10.1176/appi.ajp.161.4.692 PubMed
2. Valenstein M, Ganoczy D, McCarthy JF, et al. Antipsychotic adherence over time among patients receiving treatment for schizophrenia: a retrospective review. J Clin Psychiatry. 2006;67(10):1542–1550. doi:10.4088/JCP.v67n1008 PubMed
3. Velligan DI, Wang M, Diamond P, et al. Relationships among subjective and objective measures of adherence to oral antipsychotic medications. Psychiatr Serv. 2007;58(9):1187–1192. doi:10.1176/appi.ps.58.9.1187 PubMed
4. Zygmunt A, Olfson M, Boyer CA, et al. Interventions to improve medication adherence in schizophrenia. Am J Psychiatry. 2002;159(10):1653–1664. doi:10.1176/appi.ajp.159.10.1653 PubMed
5. Fenton WS, Blyler CR, Heinssen RK. Determinants of medication compliance in schizophrenia: empirical and clinical findings.
Schizophr Bull. 1997;23(4):637–651. doi:10.1093/schbul/23.4.637 PubMed
6. Folsom D, Jeste DV. Schizophrenia in homeless persons: a systematic
review of the literature. Acta Psychiatr Scand. 2002;105(6):404–413. doi:10.1034/j.1600-0447.2002.02209.x PubMed
7. Sajatovic M, Levin J, Fuentes-Casiano E, et al. Illness experience and reasons for nonadherence among individuals with bipolar disorder who are poorly adherent with medication. Compr Psychiatry. 2011;52(3):280–287. doi:10.1016/j.comppsych.2010.07.002 PubMed
8. West JC, Marcus SC, Wilk J, et al. Use of depot antipsychotic medications
for medication nonadherence in schizophrenia. Schizophr Bull. 2008;34(5):995–1001. doi:10.1093/schbul/sbm137 PubMed
9. Sajatovic M, Levin J, Tatsuoka C, et al. Customized adherence enhancement for individuals with bipolar disorder receiving antipsychotic therapy. Psychiatr Serv. 2012;63(2):176–178. doi:10.1176/appi.ps.201100133 PubMed
10. Sajatovic M, Levin J, Tatsuoka C, et al. Six-month outcomes of customized adherence enhancement (CAE) therapy in bipolar disorder. Bipolar Disord. 2012;14(3):291–300. doi:10.1111/j.1399-5618.2012.01010.x PubMed
11. Scott J, Pope M. Nonadherence with mood stabilizers: prevalence and predictors. J Clin Psychiatry. 2002;63(5):384–390. doi:10.4088/JCP.v63n0502 PubMed
12. Peet M, Harvey NS. Lithium maintenance, 1: a standard education programme for patients. Br J Psychiatry. 1991;158(2):197–200. doi:10.1192/bjp.158.2.197 PubMed
13. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22–33, quiz 34–57. PubMed
14. Homeless Emergency Assistance and Rapid Transition to Housing:
defining “homeless.” Fed Regist. 2011;76(233):75994–76019.
15. Haloperidol decanoate injection [package insert]. Irvine, CA: TEVA Parenteral Medicines Inc; 2009.
16. Morisky DE, Green LW, Levine DM. Concurrent and predictive validity of a self-reported measure of medication adherence. Med Care. 1986;24(1):67–74. doi:10.1097/00005650-198601000-00007 PubMed
17. Harvey NS. The development and descriptive use of the Lithium Attitudes Questionnaire. J Affect Disord. 1991;22(4):211–219. doi:10.1016/0165-0327(91)90067-3 PubMed
18. Awad AG. Subjective response to neuroleptics in schizophrenia. Schizophr Bull. 1993;19(3):609–618. doi:10.1093/schbul/19.3.609 PubMed
19. Overall JA, Gorham DR. The Brief Psychiatric Rating Scale. Psychol Rep. 1962;10(3):799–812. doi:10.2466/pr0.1962.10.3.799
20. Kay SR, Fiszbein A, Opler LA. The Positive and Negative Syndrome Scale (PANSS) for schizophrenia. Schizophr Bull. 1987;13(2):261–276. doi:10.1093/schbul/13.2.261 PubMed
21. Guy W. Clinical Global Impressions. ECDEU Assessment Manual for Psychopharmacology. Rockville, MD: US Department of Health, Education, and Welfare; 1976.
22. Morosini PL, Magliano L, Brambilla L, et al. Development, reliability and acceptability of a new version of the DSM-IV Social and Occupational Functioning Assessment Scale (SOFAS) to assess routine social functioning. Acta Psychiatr Scand. 2000;101(4):323–329. PubMed
23. Abnormal Involuntary Movement Scale. ECDEU Assessment Manual for Psychopharmacology. Rockville, MD: US Department of Health, Education, and Welfare; 1976.
24. Simpson GM, Angus JW. A rating scale for extrapyramidal side effects.
Acta Psychiatr Scand suppl. 1970;45(S212):11–19. doi:10.1111/j.1600-0447.1970.tb02066.x PubMed
25. Barnes TR. A rating scale for drug-induced akathisia. Br J Psychiatry. 1989;154(5):672–676. doi:10.1192/bjp.154.5.672 PubMed
26. Ridker PM. Fasting versus nonfasting triglycerides and the prediction of cardiovascular risk: do we need to revisit the oral triglyceride tolerance test? Clin Chem. 2008;54(1):11–13. doi:10.1373/clinchem.2007.097907 PubMed
27. Foster A, Gable J, Buckley J. Homelessness in schizophrenia. Psychiatr Clin North Am. 2012;35(3):717–734. doi:10.1016/j.psc.2012.06.010 PubMed
28. Dixon L, Weiden P, Torres M, et al. Assertive community treatment and medication compliance in the homeless mentally ill. Am J Psychiatry. 1997;154(9):1302–1304. PubMed
29. Folsom DP, Hawthorne W, Lindamer L, et al. Prevalence and risk factors for homelessness and utilization of mental health services among 10,340 patients with serious mental illness in a large public mental health system. Am J Psychiatry. 2005;162(2):370–376. doi:10.1176/appi.ajp.162.2.370 PubMed
30. Babidge NC, Buhrich N, Butler T. Mortality among homeless people with schizophrenia in Sydney, Australia: a 10-year follow-up. Acta Psychiatr Scand. 2001;103(2):105–110. doi:10.1034/j.1600-0447.2001.00192.x PubMed
31. Mortensen PB, Juel K. Mortality and causes of death in schizophrenic
patients in Denmark. Acta Psychiatr Scand. 1990;81(4):372–377. doi:10.1111/j.1600-0447.1990.tb05466.x PubMed
32. Tsuang MT, Woolson RF, Fleming JA. Premature deaths in schizophrenia and affective disorders: an analysis of survival curves and variables affecting the shortened survival. Arch Gen Psychiatry. 1980;37(9):979–983. doi:10.1001/archpsyc.1980.01780220017001 PubMed
33. Breakey WR, Fischer PJ, Kramer M, et al. Health and mental health problems of homeless men and women in Baltimore. JAMA. 1989;262(10):1352–1357. doi:10.1001/jama.1989.03430100086034 PubMed
34. Gelberg L, Linn LS, Mayer-Oakes SA. Differences in health status between older and younger homeless adults. J Am Geriatr Soc. 1990;38(11):1220–1229. PubMed
35. Osterberg L, Blaschke T. Adherence to medication. N Engl J Med. 2005;353(5):487–497. doi:10.1056/NEJMra050100 PubMed
36. Olfson M, Marcus SC, Wan GJ. Treatment patterns for schizoaffective disorder and schizophrenia among Medicaid patients. Psychiatr Serv. 2009;60(2):
210–216. doi:10.1176/appi.ps.60.2.210 PubMed
37. Zhornitsky S, Stip E. Oral versus long-acting injectable antipsychotics in the treatment of schizophrenia and special populations at risk for treatment nonadherence: a systematic review. Schizophr Res Treatment. 2012;2012:1–12. Published online Feb 15, 2012. doi:10.1155/2012/407171 PubMed
38. Hughes DA. Estimation of the impact of noncompliance on pharmacokinetics: an analysis of the influence of dosing regimens.
Br J Clin Pharmacol. 2008;65(6):871–878. doi:10.1111/j.1365-2125.2008.03124.x PubMed
39. Ereshefsky L, Mascarenas CA. Comparison of the effects of different routes
of antipsychotic administration on pharmacokinetics and pharmacodynamics. J Clin Psychiatry. 2003;64(suppl 16):18–23. PubMed
40. Fleischhacker WW, Meise U, Günther V, et al. Compliance with antipsychotic drug treatment: influence of side effects. Acta Psychiatr Scand suppl. 1994;382:
11–15. PubMed
41. Cañas F, Möller HJ. Long-acting atypical injectable antipsychotics in the treatment of schizophrenia: safety and tolerability review. Expert Opin Drug Saf. 2010;9(5):683–697. doi:10.1517/14740338.2010.506712 PubMed